Introduction
Calcific tendinitis is a relatively common disorder, caused by the excessive depositing of calcium hydroxyapatite crystals in the tendons. It typically affects patients between the third and sixth decades of life, with a higher prevalence in females. The joints most commonly involved in this disorder are the shoulder and hip(1). Calcific tendinitis in the proximity of the coxofemoral joint accounts for 5.4% of all cases in individuals over 15 years of age, occurring most frequently in the tendons of the rectus femoris and gluteus medius(2). The initial treatment of calcific tendinitis consists of oral nonsteroidal antiinflammatory drugs, physiotherapy, image-guided corticosteroid infiltration, high-intensity focused ultrasound, percutaneous ultrasound-guided barbotage, and shockwave therapy(3). The main indication for surgery is in cases that prove refractory to conservative treatment, with symptoms that limit the activities of daily living.
There is a significant number of articles in the literature on the endoscopic treatment of calcific tendinitis of the gluteus medius. In contrast, there is not much evidence on the surgical treatment of calcific tendinitis of the gluteus maximus. In an exhaustive literature search, we found only one article (a case report) describing endoscopic treatment for this condition(4). The present study describes a case of calcific tendinitis of the gluteus maximus successfully treated by endoscopic surgery.
Clinical case
The patient was a 46-year-old woman presenting chronic pain for the past three years, with an insidious onset, located in the posterolateral area of the right hip, at the level of the insertion of the gluteus maximus tendon. In addition, she reported radiculopathy in the right lower limb, with dysesthesia.
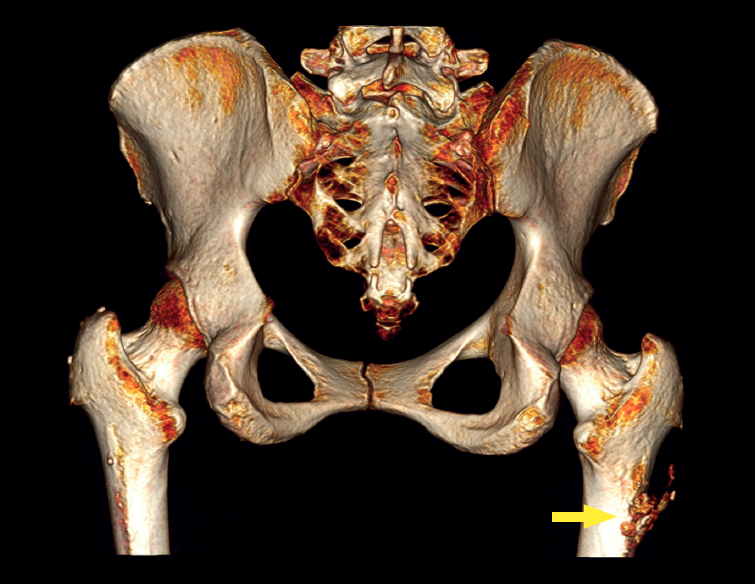
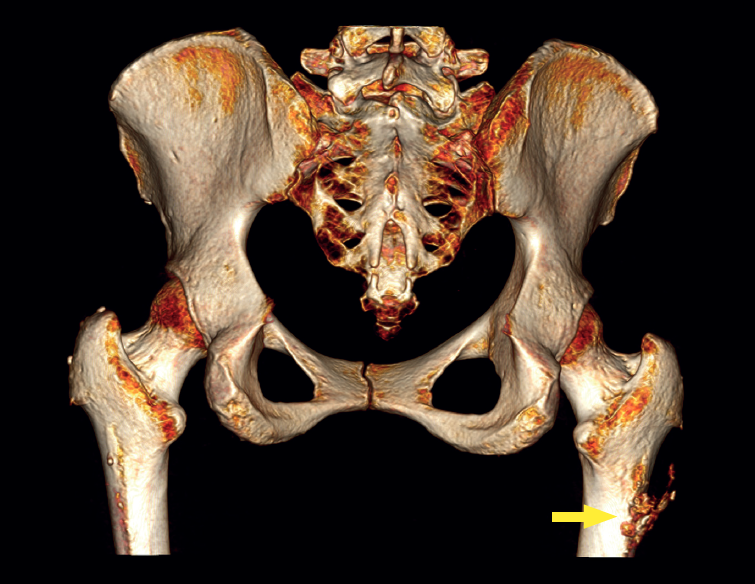
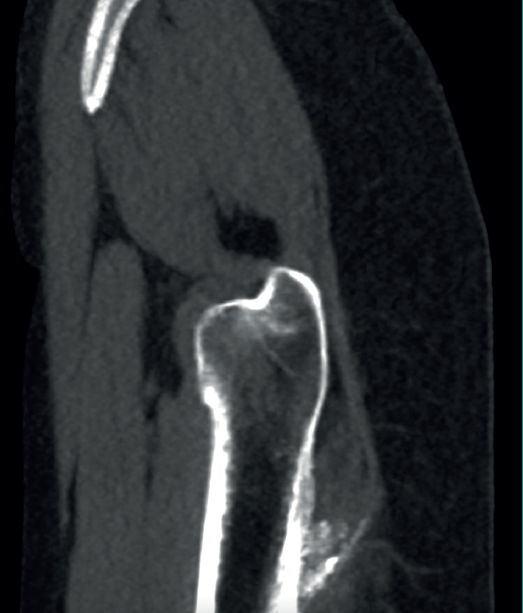
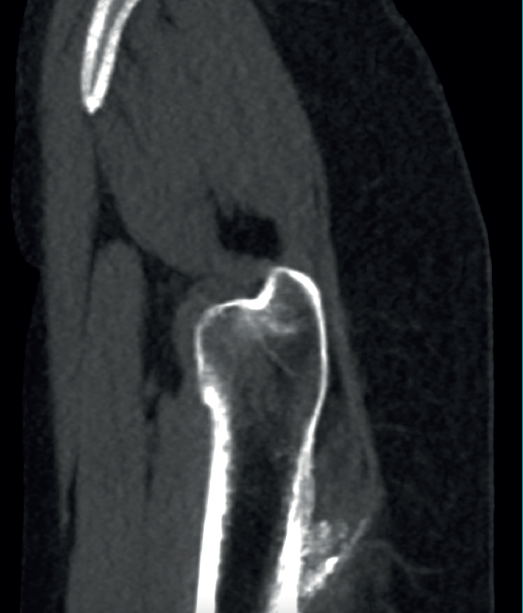
The physical examination revealed a limp-free gait and complete joint balance, with no positive signs of femoroacetabular impingement or inguinal pain. Muscle strength was preserved and similar to that of the contralateral side. She experienced intense pain on palpation of the insertion of the gluteus maximus, referred proximally to the ipsilateral buttock. The pain was reproduced on extension against resistance, and prevented sitting for long periods. Plain radiographic and computed tomography (CT) images revealed calcific tendinosis affecting the aponeurotic prolongation of the gluteus maximus in proximity to its insertion in the upper region of the linea aspera of the femur (Figures 1 and 2) Magnetic resonance imaging (MRI) of the hip showed a labral tear, that proved asymptomatic in the physical examination. In view of the clinical picture of radicular pain, an MRI scan of the lumbar spine and subgluteal space was also performed, ruling out radicular involvement or sciatic neuritis. Her previous treatment over the three years of evolution of the disorder included oral nonsteroidal anti-inflammatory drugs, a specific physiotherapy programme and several ultrasound-guided corticosteroid injections with positive results - though a last session showed no response. Due to the severity and chronicity of the symptoms and their resistance to conservative treatment, surgery was decided to clean and remove the intratendon calcification endoscopically.
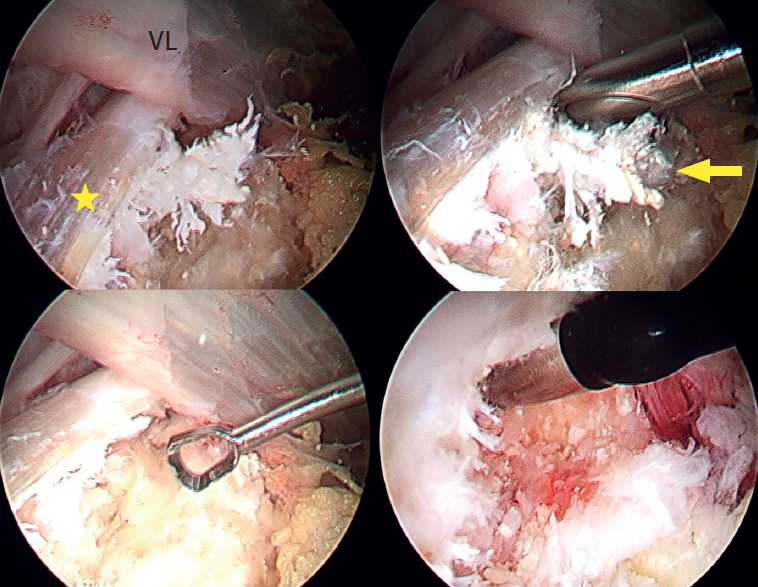
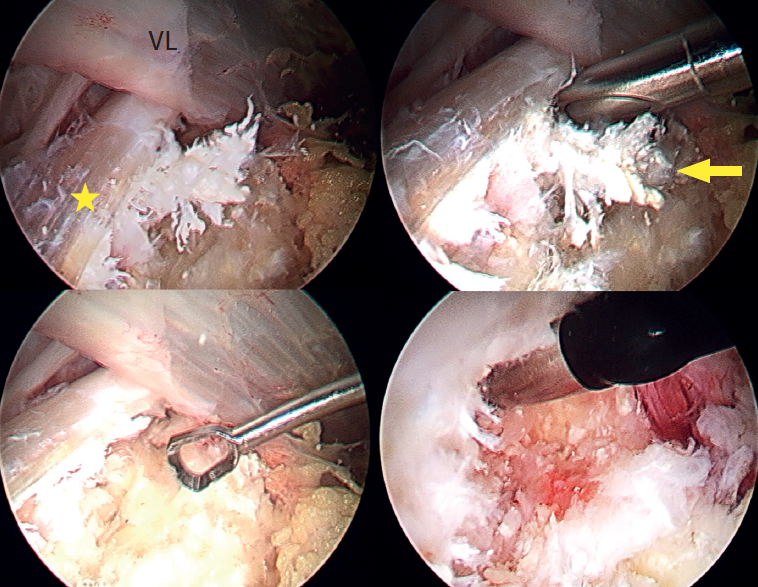
Under combined (spinal and general) anaesthesia, the patient was placed on the traction table in supine decubitus with the contralateral leg in abduction. The hip to be operated upon was placed in 10-15ºflexion with slight approximation towards the neutral midline. The hip was minimally distracted by the longitudinal traction combined with pressure from a perineal post, and the foot of the leg to be operated upon was internally rotated to bring the femoral neck parallel to the floor, tilting the table 10° towards the opposite side. The calcification was then located using fluoroscopy, and two portals were created in the peritrochanteric space using the all inside technique. The first (vision) portal was located at the level of the vastus crest in the area of the modified anterior portal, and the second (working) portal was located distal and anterolateral at the level of the calcification. A trochanteric bursectomy was performed to visualise the gluteus maximus tendon and, once the latter was located, the calcification was identified, characterised by a whitish colour with a coral-like appearance and pasty consistency, and then removed using motorised instruments, curette and radiofrequency (Figure 3). Finally, the integrity of the tendon was checked, and complete removal of the calcification was confirmed under visual control. Postoperatively, a nonsteroidal antiinflammatory drug (naproxen) was prescribed for three weeks as prophylaxis for heterotopic ossifications.
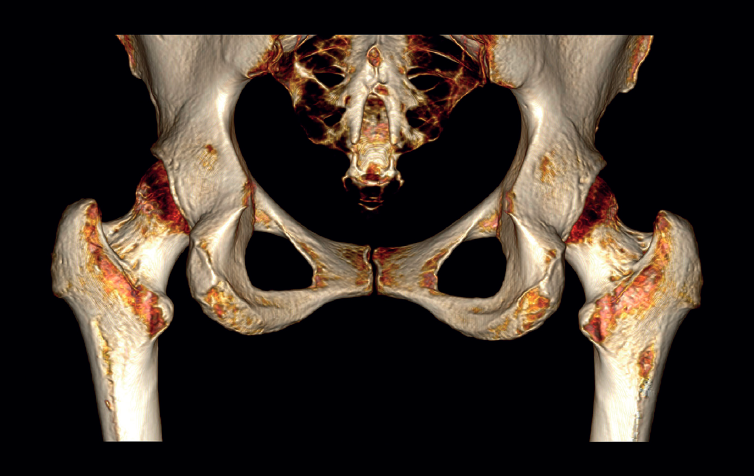
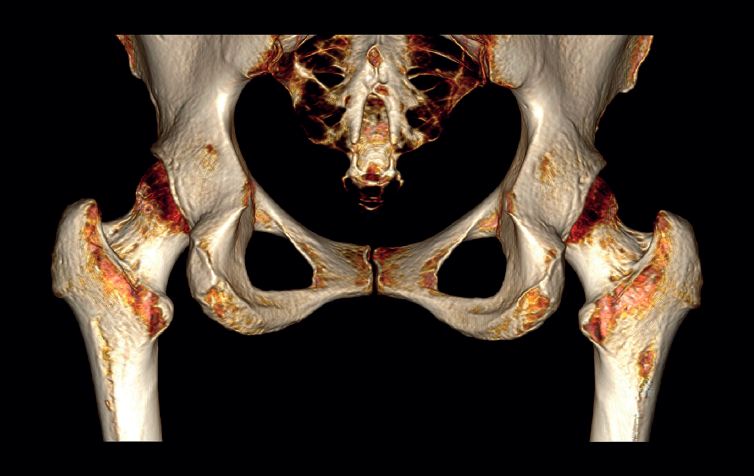
A usual rehabilitation protocol after hip arthroscopy / endoscopy was applied, with crutch-assisted weight bearing for three weeks and circumduction movements plus stationary cycling for 15 minutes, four times a day. The patient was advised to avoid extension and long stride exercises in order to prevent possible gluteus maximus tendon injuries. She reported complete reversal of the symptoms, including the radicular pain, with a return to physical activity and sports three months after surgery. One year after the operation, the patient remained asymptomatic in any activity, with complete disappearance and no recurrence of the calcification (Figure 4).
Discussion
Calcific tendinitis evolves in different phases, each characterised by specific radiological images and symptoms. The disorder begins with the formative phase, in which a region of the tendon, for an unknown reason, undergoes fibrocartilaginous transformation. This is followed by a calcification phase that may cause pain of mechanical characteristics. The next phase is the resorptive phase, characterised by peripheral neovascularisation and the migration of macrophages that absorb the calcium deposit. This is the stage of greatest pain intensity. Finally, in the reabsorption phase, the fibroblasts restore the normal pattern of the tendon(1). The hip is the second most common joint affected by calcific tendinitis. The tendons most frequently involved are those of the rectus femoris (the direct head more than the indirect head of the muscle). These are followed by the gluteal tendons (with a greater prevalence of the medius over the maximus) and, to a lesser extent, other tendons such as those of the adductors, the piriformis, the iliopsoas, the ischiotibial and the sartorius muscles.
Depending on the tendon affected, the differential diagnosis includes various conditions: infections, tumours (such as parosteal osteosarcoma), lumbar radiculopathy, avulsion fracture, myositis ossificans, os acetabuli or sesamoid bones(5).
In terms of anatomy, the gluteus maximus originates from the posterior gluteal line, the posterior surface of the sacrum and coccyx, and the sacrotuberous ligament. Its upper fibres insert into the iliotibial band, and the lower fibres insert into the linea aspera of the femur. This muscle is innervated by the inferior gluteal nerve (L5, S1 and S2). Its actions are thigh extension and external rotation of the femur(5).
Calcific tendinitis of the gluteus maximus typically occurs in the fibres that insert on the posterolateral aspect of the femur(8). With regard to the clinical features of calcific tendinitis of the gluteus maximus, the pain usually has an insidious onset with periods of exacerbation related to physical activity. The acute symptoms, understood as lasting less than three weeks, are related to larger initial lesions, and are more prevalent in young patients. The symptomatology in such cases is of greater intensity and recovery is more satisfactory compared to patients with chronic symptoms. Calcifications with delimited margins respond better to treatment than lesions with irregular margins(9).
On physical examination, hip range of motion is full, painless and symmetrical to the contralateral side. Moreover, muscle strength is usually preserved and walking is usually normal, though antalgic gait may be observed. Of note is intense pain on palpation in the affected buttock and over the femoral insertion of the gluteus maximus tendon, distal to the trochanteric bursa(10,11). Cases of sciatic pain together with a positive neural tension test (seated slump test)have also been described(8,12,13). In these cases the differential diagnosis should be made with so-called deep gluteal syndrome, a syndrome characterised by pain and/or dysesthesia in the buttock, hip or posterior thigh, together with radicular pain due to impingement of the sciatic nerve, which is located posterior to the insertion of the gluteus maximus at a distance of 3-6 cm, in the subgluteal space. One of the causes of this is compressive fibrous bands running between the posterior surface of the greater trochanter and the gluteus maximus(14,15,16).
In cases of calcific tendinopathy of the gluteus maximus, calcifications in the femoral metaphysis can be seen on plain radiographs, though a normal image may also be seen. Therefore, CT and/or MRI scans are usually necessary for establishing the diagnosis, exhibiting an irregularity or cortical erosion at the insertion of the gluteus maximus in the gluteal tuberosity, located on the posterolateral surface of the femur, distal to the greater trochanter, accompanied by areas of tendon calcification, local inflammatory signs and, in some cases, partial intratendinous ruptures(17). Use can also be made of CT-guided single-photon emission computed tomography (SPECT-CT), which pinpoints the anatomical location and assesses the activity of the lesion, and is of interest in the differential diagnosis in oncological patients(18).
Regarding the treatment of calcific tendinitis and specifically concerning the aforementioned disorder of the gluteus maximus tendon, the initial indication is conservative treatment, based on the prescription of oral nonsteroidal antiinflammatory drugs and physiotherapy. Sang-Min Park et al. reported that in 66% of the cases, the symptoms caused by calcific tendinitis were resolved within 2.5 months, without the need for any interventional technique or surgery(3). In patients who do not respond to conservative treatment, techniques such as imaging-guided corticosteroid infiltration, high-intensity focused ultrasound, percutaneous ultrasound-guided barbotage, and shockwave therapy are indicated. Hema Nalini Choudur et al. described imaging-guided (fluoroscopy or CT) corticosteroid-anaesthesia infiltration in these cases, achieving a return to daily activities in all patients, with complete resolution of the pain within a maximum period of 6 months(19). Hannae Jo et al. described percutaneous ultrasound-guided barbotage in a patient where conservative treatment and shock wave therapy had been ineffective - achieving both symptoms relief and resolution of the calcification on the radiographs(13). Kwang-Jun Oh et al. used shockwave therapy for the treatment of calcific tendinitis around the hip, achieving optimal clinical and radiological outcomes with a follow-up period of 15 months(20). Champ L. Baker et al. described percutaneous ultrasound-guided tenotomy for gluteal tendinopathy, achieving pain relief and functional improvement as assessed by validated questionnaires, with no reported complications(21).
Surgery is indicated in cases where both conservative treatment and the techniques described above prove ineffective and the symptoms limit the activities of daily living of the patient. Manoj Kumar et al. presented a case of calcific tendinitis of the gluteus maximus treated by open surgery with a large incision size and extensive soft tissue dissection(8). Ariel A. Williams et al. in turn described a similar case in a golfer. The authors performed open surgery involving debridement of the tendinosis and repair of the tendon using sutures with anchorings(10). Regarding the endoscopic technique, most of the published articles refer to the treatment of calcific tendinitis of the gluteus medius. In 2003, Utku Kandemir et al. reported the first case of calcific tendinitis of the gluteus medius and minimus subjected to endoscopic surgery, recommending this technique due to its effectiveness and low morbidity(22). Subsequently, Chen Jean et al. and Lee Wen Qiang et al. successfully reproduced this endoscopic debridement technique in similar patients(23,24). Justin J. Mitchell et al. described the endoscopic surgical technique for trochanteric bursectomy and iliotibial band lengthening for the treatment of trochanteric bursitis. Although such surgery is technically demanding, it offers complete visualisation of the trochanteric bursal space, as well as certain advantages over the open technique: minimal incisions, less soft tissue dissection and reduced blood losses(25).
In 2021, Charles A. Su et al. published for the first time an article on the endoscopic treatment of calcific tendinitis of the gluteus maximus involving trochanteric bursectomy and debridement of the calcification in a manner similar to that described in this case(4). The use of nonsteroidal antiinflammatory drugs to prevent postoperative calcifications was published by Randelli in arthroscopic hip surgery, evidencing high efficacy(26). The present study describes the second case of calcific tendinitis of the gluteus maximus treated by endoscopic surgery, considering it to be a reproducible and effective technique.
Conclusions
Endoscopic surgery for calcific tendinitis of the gluteus maximus allows controlled excisional debridement under direct vision, with the additional advantages of less morbidity, smaller incisions, less soft tissue injury (including a lesser risk of sciatic nerve problems thanks to the direct and magnified vision), less blood loss, a shorter exposure time and therefore less risk of infection, and much faster recovery compared with open surgery.